I found this describing testing. Molecular testing seems to be the most accurate.
What are the different types of tests to diagnose COVID-19?
Yale Medicine experts explain the ins and outs of lab- and home-based tests.

www.yalemedicine.org
You copied in full a post I made a few posts up (the substack from Dr, Alexander is in post 63,675, the 2nd to last post I made last night), but have left a few links without any content, such as this one! Please try to post all the articles you link to (it's actually a rule for TB, no blind links, but I don't think this thread is read by the Mods/Admin so you've been lucky!). For two reasons. Some are reading on phones or on limited bandwith and it's harder to open a new window, and also because sometimes things disappear so we have it archived here.

If you aren't able to, you can pm me the link and I'll post it at your request (as I do for Profit of Doom, whose links introduced me to substack a few months back for which I am extremely grateful).
Yale Medicine experts explain the ins and outs of lab- and home-based tests.

www.yalemedicine.org
(fair use applies)
Which COVID-19 Test Should You Get?
BY
CARRIE MACMILLAN
January 20, 2022
Yale Medicine experts explain the ins and outs of lab- and home-based tests.
[Originally published: Oct. 20, 2021. Updated: Jan. 20, 2022.]
Note: Information in this article was accurate at the time of original publication. Because information about COVID-19 changes rapidly, we encourage you to visit the websites of the Centers for Disease Control & Prevention (CDC), World Health Organization (WHO), and your state and local government for the latest information.
As the highly contagious
Omicron variant continues to sweep across the country, people—even those who are fully vaccinated—are wondering if the onset of cold and
flu symptoms is really a sign of
COVID-19 infection.
But COVID testing has become a complicated issue. As Omicron surged, appointments at sites where results are processed by a laboratory became difficult to find in a timely manner. So, many turned to at-home COVID-19 tests. Often called rapid tests, such kits are sold in drugstores and online, allowing people to test themselves—and get results—in their own home in a matter of minutes.
Unfortunately, at-home tests have also become difficult—if not impossible—to find. The federal government hopes to alleviate the bottleneck by requiring private insurance companies to start reimbursing customers for at-home tests and by distributing 1 billion free rapid tests to Americans.
If you can get your hands on a test, you might find the different options confusing. In which situations is a laboratory-based (often called PCR) test best? If you are traveling and need to show a negative COVID test, which should you get? Are they all equally accurate? Do some produce results faster than others? And how far does that Q-tip go up your nose with each kind?
Some of these questions are easy to answer, while others are more difficult—particularly when it comes to accuracy. That’s because all of the tests—and there are hundreds of them, from a growing number of companies and laboratories—are offered through a Food and Drug Administration (FDA) emergency use authorization (EUA). Therefore, they have not been as rigorously tested or vetted as other medical tests with full FDA approval.
And since the virus is new, all the tests are also new, meaning we have neither a long track record of comparing results, nor a true gold-standard test yet.
Furthermore, with each new
variant, new questions arise. Recently, there has been discussion about whether throat swabs or saliva samples are better at detecting Omicron compared to the more mainstream method of nasal swabs—or if rapid tests are less effective at detecting Omicron.
Sheldon Campbell, MD, PhD, a Yale Medicine pathologist and microbiologist, cautions against getting caught up in what he calls mostly anecdotal data.
“There is some PCR-based data that saliva is better, but the home tests are designed to work with a nasal swab and very few responsible people would think you should replace a nasal swab with a throat swab. That’s Twitter medicine,” says Dr. Campbell, referring to a #swabyourthroat hashtag that is trending. “And I have not seen good data that antigen tests are somehow less sensitive with Omicron than they are with other strains.”
Below, Dr. Campbell and Yale Medicine infectious disease experts get into the nuances of the various available COVID-19 tests.
What are the different types of tests to diagnose COVID-19?
Unlike antibody tests, which look for prior infection, COVID diagnostic tests look for current infection with SARS-CoV-2, the virus that causes
COVID-19. They are broken into two categories: molecular and antigen (more below).
A summary of their differences
Because the samples are, for the most part, collected in the same way for both, the differences between the two kinds of tests are largely in how they’re processed.
Molecular tests are generally more accurate and mostly processed in a laboratory, which takes longer; antigen tests—or “rapid tests”—are processed pretty much anywhere, including at home, in doctors’ offices, or in pharmacies. You can get antigen test results in about 15 minutes, but they tend to be less accurate.
Health care providers typically rely on molecular tests, particularly when people have COVID-19 symptoms, whereas antigen testing is often used when quick results are needed or for general screening and surveillance.
Below, we take a closer look at the two categories.
Molecular COVID tests (also called nucleic acid amplification test, or NAAT)
The first test created to detect COVID—and still the most widely used—is a molecular test called PCR (polymerase chain reaction), Dr. Campbell says. “PCR and similar tests look for the COVID virus’s RNA,” meaning genetic material that comes only from the virus, he explains. “They tend to be quite sensitive, but even among these, they are on a continuum of sensitivity and vary a whole lot.”
“Sensitivity” measures how often a test correctly delivers a positive result for people with the condition that's being tested. A test that's highly sensitive will catch almost anyone who has the disease and not generate a lot of false-negative results.
How does the test work? A molecular test looks for genetic material from the virus. The test uses sophisticated chemicals and equipment to reproduce millions to billions of copies of viral-related DNA from even the smallest sample. Because of that, the test is considered highly sensitive, leading to very few false negatives.
How is a sample obtained? Usually with a swab inserted into your nose. There are three different methods for nasal collection:
- Nasopharyngeal: A health care professional inserts a long swab deep into your nostril to collect fluid from the back of your nose.
- Mid-turbinate: This method, which someone can be coached to do themselves or is done by a professional, involves placing a soft swab straight back into the nostril (less than one inch) to collect a sample.
- Anterior nasal swab: This test, which can either be self-administered and possibly supervised by a trained health care provider, or done by a health care professional, involves putting a swab three-quarters of an inch into the nostril and twirling it around at least four times to get a sample.
In general, the deeper you go for a specimen, the greater the sensitivity, says
Richard Martinello, MD, a Yale Medicine infectious disease expert. “But, we’ve found it’s much more comfortable to do mid-turbinate or anterior nasal swabs, and they provide a reasonable degree of sensitivity,” he adds. “It’s a compromise of sorts, but it does allow us to simplify the collection process.”
Other collection methods include:
- Oropharangeal (throat) swab: A trained health care provider collects a sample using a swab to the back of the throat.
- Saliva: You drool into a sterile, leak-proof cap container. For now, this type of testing is only offered at select locations.
How is the test processed? Most specimens are sent to laboratories.
Where can you get one? Molecular tests are offered at pharmacies, doctors' offices, and designated testing locations, such as health clinics, as well as locations set up by private or state and local public health systems.
How quickly can you get results? Because the tests are sent to a lab, it depends on lab capacity. Results are typically available within a range of one to seven days, depending on your location.
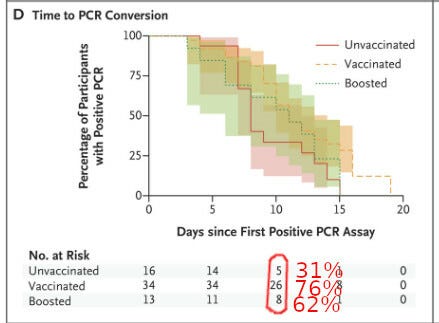
“Currently, Yale New Haven Health System is turning around about 76% of community test results within 24 hours and just over 95% within 48 hours,” says
Scott Roberts, MD, a Yale Medicine infectious disease specialist.
How accurate are they? According to the Centers for Disease Control and Prevention (CDC), laboratory-based tests, such as PCR, have a “generally high” test sensitivity.
“PCR tests are considered the most accurate available,” Dr. Martinello says. “But because these tests are highly sensitive and specific, there is still a risk for a false positive.”
But limiting false
negatives might be extremely important, especially with the rise of more transmissible variants. "It’s actually true for those who have—and who don’t have—symptoms, but if you
do have symptoms, a PCR test is more likely than an antigen test to pick up an infection accurately,” says Dr. Campbell.
Antigen COVID tests
Whereas molecular tests require specialized equipment for processing samples, an antigen test is simpler, because it requires smaller devices that are easy to transport. Their design is similar to, say, a pregnancy test.
How does the test work? Antigen tests search for pieces of protein from the SARS-CoV-2 virus. The sample you provide is treated with a reagent and analyzed on the spot by a health care professional. Unlike molecular tests, these require a higher level of virus in the test sample before the test will turn positive. This means that an antigen test may sometimes lead to a false negative.
How is a sample obtained? As with molecular tests, a sterile swab is inserted into your nose or throat to obtain a specimen (see details above)—although throat swabs may be less common these days.
How is the test processed? The sample is self-applied to a test strip or cartridge. Similar to a home pregnancy test, results show a colored line to signify positive or negative.
Where can you get one? Antigen tests are offered in pharmacies, doctors' offices, and can be purchased to use at home.
How quickly can you get results? Results are typically available in 10 to 15 minutes.
How accurate are they? According to the CDC, antigen test sensitivity varies depending on the time in the course of one’s infection, but is considered to have “moderate to high” sensitivity during peak viral load. Compared to molecular tests, antigen tests are more likely to generate false negative results, especially when performed on people who don’t have symptoms.
ID NOW COVID Test
Complicating things a bit is the availability of ID NOW, a rapid
molecular test used by some testing locations, such as pharmacies, that can read results on-site—in about 15 minutes.
According to the CDC, point-of-care tests (such as those administered at a drug store, including ID NOW), have a “moderate to high” test sensitivity.
But where does it fit in the molecular vs antigen test result accuracy spectrum?
“ID NOW is not a completely different thing than PCR, it’s just on the lower sensitivity end of the spectrum,” Dr. Campbell says. “So, more accurate than an antigen test.”
[continued next post]








 If you aren't able to, you can pm me the link and I'll post it at your request (as I do for Profit of Doom, whose links introduced me to substack a few months back for which I am extremely grateful).
If you aren't able to, you can pm me the link and I'll post it at your request (as I do for Profit of Doom, whose links introduced me to substack a few months back for which I am extremely grateful).
















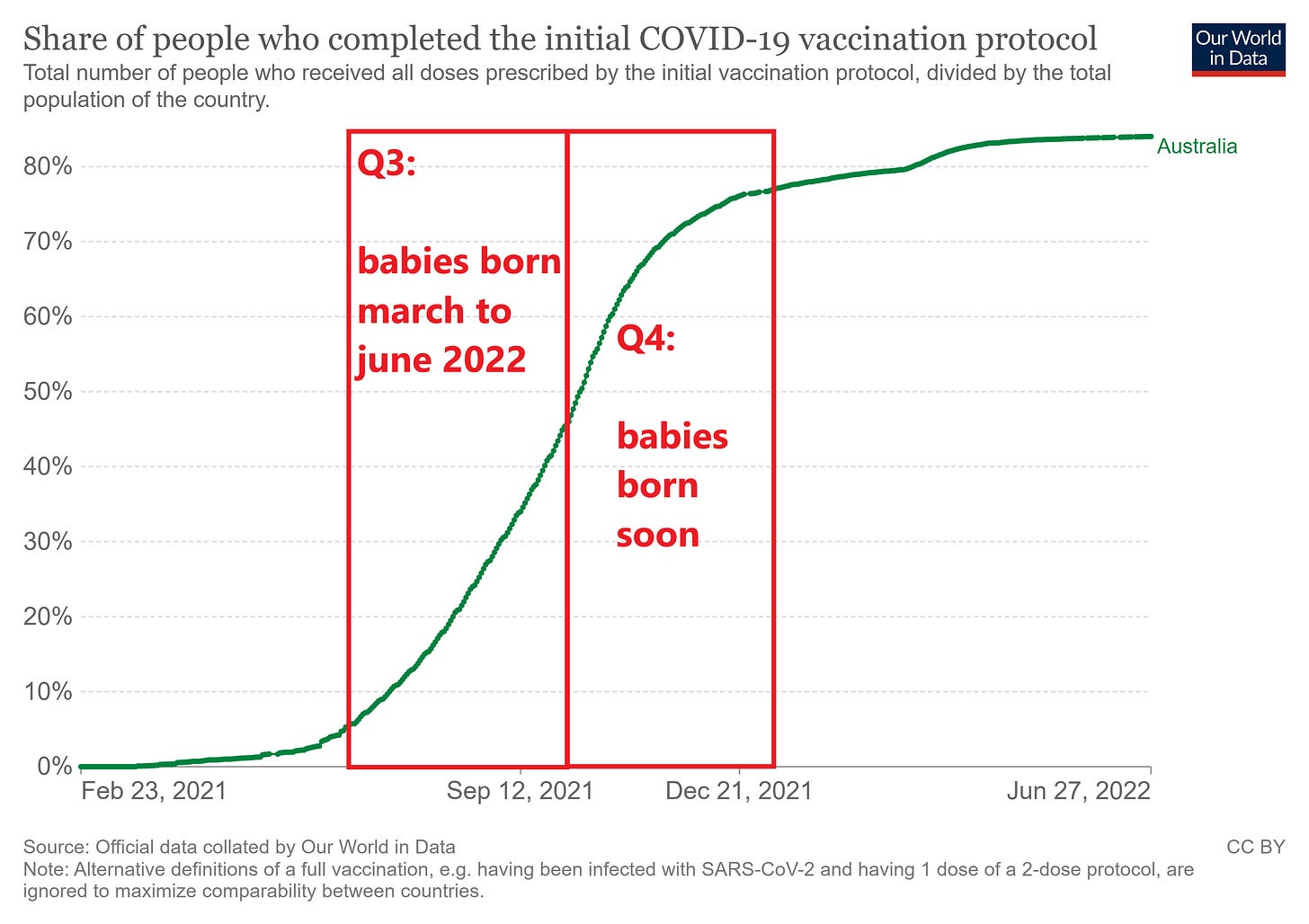
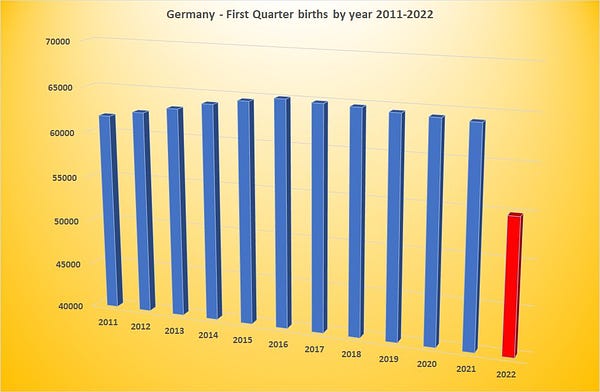
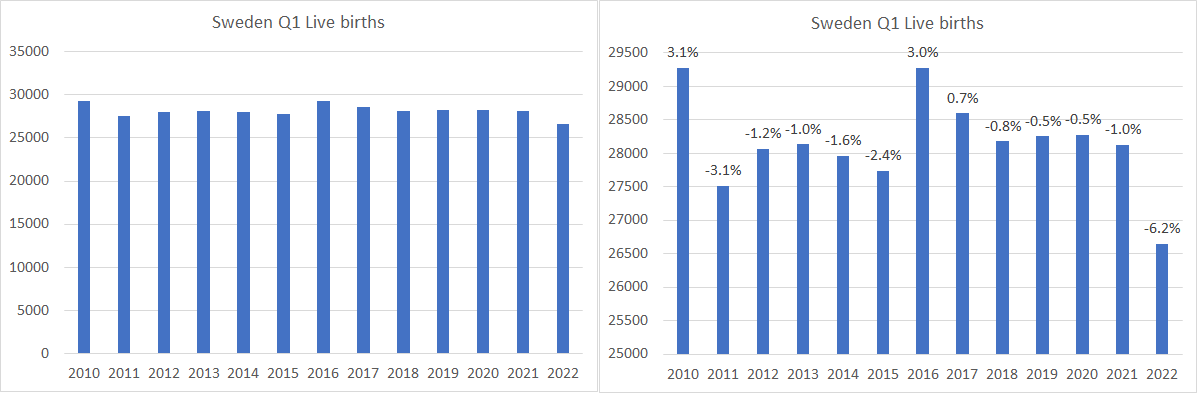
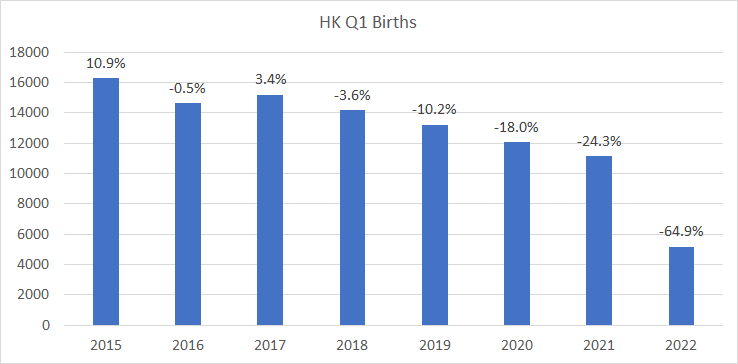
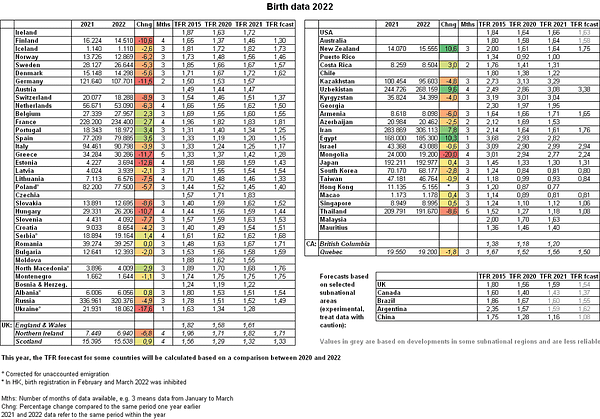
 Depopulation of TaiwanBirth Rate Dropped by 23% in ONE YEAR -- And it is NOT Covidigorchudov.substack.com
Depopulation of TaiwanBirth Rate Dropped by 23% in ONE YEAR -- And it is NOT Covidigorchudov.substack.com